The Deadly Side of Valley Fever
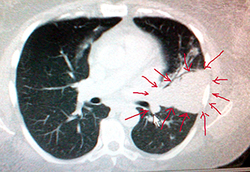 Chest CT Scan of Cocci Tumor
Chest CT Scan of Cocci Tumor
By Sharon Weltz
Most Arizonan’s have heard about the mild form of Valley Fever that consists of flu-like symptoms and fatigue. But few are aware of a potentially deadly form of Valley Fever. Almost 6,000 cases were reported in the Valley last year, and there will likely be another 6,000 this year. Follow these simple steps to help protect yourself from this potentially deadly form of Valley Fever, Disseminated Coccidioidomycosis (or Cocci, for short.)
What is Cocci?
Coccidioides immitis is a microscopic spore that lives in the dirt, and is endemic to two regions of the United States: the Arizona Desert and California desert. Cocci spores enter the human body by being inhaled into the lungs. Most people’s immune system can fight off a few odd spores now and again. But inhaling large amounts of Cocci spores overwhelms even the best immune system. When this happens, Cocci spores grow and morph from individual microscopic spores into a solid, growing mass of cells. This growing mass takes up more and more space, reducing lung function. As weeks go by, Cocci is carried through the bloodstream and attacks other parts of the body.
Symptoms
Early stage symptoms appear 1-3 weeks after inhaling the spores: Increasing fatigue, fever, cough, and chest pain that does not get better with antibiotics. Soon, additional symptoms begin to manifest: joint pain, skin lesions, drenching night sweats, vision problems, thrush, shortness of breath, muscle pain and weakness, weight loss, and eventually Meningitis. The disease is so little known and incapacitating that Cocci was once listed as an approved agent for biological warfare. It was never used, but just imagine dropping a few payloads of Cocci infested dust on the enemy. Those infected could be bedridden within a month.
Diagnosis and Testing
Cocci is often misdiagnosed as bronchitis or pneumonia, and this delay allows it to spread unabated throughout the body. Those who experience symptoms of increased fatigue, cough and fever should be proactive: demand to be tested for Valley Fever. The Center for Disease Control (CDC) recommends that doctors treating patients living in endemic regions who display flu-like or pneumonia-like symptoms be tested for Valley Fever upon their first examination.
An x-ray is not enough: Pneumonia looks the same as Valley Fever in a chest x-ray. To be diagnosed, a blood test to measure Cocci titers must be taken. Blood test results take 2 weeks, so the sooner you are tested and correctly diagnosed, the sooner you can begin the correct drug therapy. While waiting for the test results, doctors often prescribe antibiotics to treat symptoms. But if you do have Valley Fever, your symptoms will increase, since antibiotics have no effect.
The Cure
At the present time, there is no specific cure. To overcome the disease, steps are taken to slow or stop the spread of the disease with the help of high doses of antifungal medication. Cocci is a fungus, and antifungal medications create a hostile environment for the fungus. The antifungal medication works like a football line backer – it slows or holds the opposition back so you can advance, allowing your body’s immune system to work at eliminating the fungus. But it takes months, sometimes years, to eliminate Cocci from your body, and a few people die every year from complications associated with the disease.
The good news is that the CDC is fast-tracking a vaccine, developed at the University of Arizona, which will protect people and animals from contracting the disease (you’ll want to vaccinate your dog, too, when the vaccine becomes available.) You can read more about that here.
How to Protect Yourself
You cannot catch Cocci from another person. You catch it by inhaling dust. If you are gardening and raising dust; If you are in the vicinity of a leaf blower; If you are driving through billowing clouds of dust raised by field plowing; If a dust storm is coming … don’t inhale the dust. Use these tips to decrease your chances of inhaling Cocci spores:
· During dust storms, stay indoors and keep windows and doors closed.
· Driving through dust? Keep car windows and vents closed to keep dust out.
· Wear an N95 rated mask to protect yourself from Cocci spores lurking in rising, billowing, or moving dust. N95 masks are available for purchase from most drug and hardware stores, and online.
Final Word: My Personal Battle with Cocci
In the early days of November 2014, following a 3-week backyard gardening project that produced raised dust clouds, I began feeling run-down, and a severe fatigue set in. Over a two-week period I developed a cough and fever. I was first diagnosed with bronchitis, and when antibiotics had no effect, a chest ex-ray was taken. I was diagnosed with pneumonia, and was prescribed a stronger antibiotic.
My health continued to decline, so a higher dose of the antibiotic was prescribed. By this time my symptoms included cough, fever, nausea, vomiting, drenching night sweats, skin lesions, joint and muscle pain, vision fluctuations, extreme fatigue, and muscle weakness. It hurt to bathe. It hurt to wear shoes. It hurt to be touched on my arms and legs. I did not have enough breath to speak a single sentence.
A chest CT scan was ordered, which revealed a mass in my left lung.
My doctor referred me to a pulmonary specialist, and ordered the Cocci titers blood test. Two weeks later the test results were in: I had Disseminated Coccidioidomycosis.
I sought out a local Valley Fever specialist. “Every Valley Fever patient’s rate of recovery is different,” said Dr. Craig Rundbaken, of the Respiratory & Valley Fever Clinic. The new plan of attack involved anti-fungal drugs, monthly titer and liver tests (the medication is hard on your liver,) chest x-rays, and plenty of rest.
Healing is a slow process. It’s been 8 months since my Valley Fever was diagnosed, and progress is good: many symptoms have disappeared, the mass in my lung has shrunk to 4.9cm (about 2 inches), and my blood titer levels continue to decline.
Want to know more?
The CDC website offers Valley Fever information.
The book, Valley Fever Silent Epidemic: The Common, Often Misdiagnosed Desert Ailment, by local expert Dr. Craig Rundbaken, offers information for both patients and healthcare professionals.
A YouTube channel is dedicated to sharing information about Valley Fever. You can watch the videos here.
An excellent paper on the Cocci spore, where it lives, and when it is most active, was written by Tom Volk of the University of Wisconsin. You can read his report online.
Most Arizonan’s have heard about the mild form of Valley Fever that consists of flu-like symptoms and fatigue. But few are aware of a potentially deadly form of Valley Fever. Almost 6,000 cases were reported in the Valley last year, and there will likely be another 6,000 this year. Follow these simple steps to help protect yourself from this potentially deadly form of Valley Fever, Disseminated Coccidioidomycosis (or Cocci, for short.)
What is Cocci?
Coccidioides immitis is a microscopic spore that lives in the dirt, and is endemic to two regions of the United States: the Arizona Desert and California desert. Cocci spores enter the human body by being inhaled into the lungs. Most people’s immune system can fight off a few odd spores now and again. But inhaling large amounts of Cocci spores overwhelms even the best immune system. When this happens, Cocci spores grow and morph from individual microscopic spores into a solid, growing mass of cells. This growing mass takes up more and more space, reducing lung function. As weeks go by, Cocci is carried through the bloodstream and attacks other parts of the body.
Symptoms
Early stage symptoms appear 1-3 weeks after inhaling the spores: Increasing fatigue, fever, cough, and chest pain that does not get better with antibiotics. Soon, additional symptoms begin to manifest: joint pain, skin lesions, drenching night sweats, vision problems, thrush, shortness of breath, muscle pain and weakness, weight loss, and eventually Meningitis. The disease is so little known and incapacitating that Cocci was once listed as an approved agent for biological warfare. It was never used, but just imagine dropping a few payloads of Cocci infested dust on the enemy. Those infected could be bedridden within a month.
Diagnosis and Testing
Cocci is often misdiagnosed as bronchitis or pneumonia, and this delay allows it to spread unabated throughout the body. Those who experience symptoms of increased fatigue, cough and fever should be proactive: demand to be tested for Valley Fever. The Center for Disease Control (CDC) recommends that doctors treating patients living in endemic regions who display flu-like or pneumonia-like symptoms be tested for Valley Fever upon their first examination.
An x-ray is not enough: Pneumonia looks the same as Valley Fever in a chest x-ray. To be diagnosed, a blood test to measure Cocci titers must be taken. Blood test results take 2 weeks, so the sooner you are tested and correctly diagnosed, the sooner you can begin the correct drug therapy. While waiting for the test results, doctors often prescribe antibiotics to treat symptoms. But if you do have Valley Fever, your symptoms will increase, since antibiotics have no effect.
The Cure
At the present time, there is no specific cure. To overcome the disease, steps are taken to slow or stop the spread of the disease with the help of high doses of antifungal medication. Cocci is a fungus, and antifungal medications create a hostile environment for the fungus. The antifungal medication works like a football line backer – it slows or holds the opposition back so you can advance, allowing your body’s immune system to work at eliminating the fungus. But it takes months, sometimes years, to eliminate Cocci from your body, and a few people die every year from complications associated with the disease.
The good news is that the CDC is fast-tracking a vaccine, developed at the University of Arizona, which will protect people and animals from contracting the disease (you’ll want to vaccinate your dog, too, when the vaccine becomes available.) You can read more about that here.
How to Protect Yourself
You cannot catch Cocci from another person. You catch it by inhaling dust. If you are gardening and raising dust; If you are in the vicinity of a leaf blower; If you are driving through billowing clouds of dust raised by field plowing; If a dust storm is coming … don’t inhale the dust. Use these tips to decrease your chances of inhaling Cocci spores:
· During dust storms, stay indoors and keep windows and doors closed.
· Driving through dust? Keep car windows and vents closed to keep dust out.
· Wear an N95 rated mask to protect yourself from Cocci spores lurking in rising, billowing, or moving dust. N95 masks are available for purchase from most drug and hardware stores, and online.
Final Word: My Personal Battle with Cocci
In the early days of November 2014, following a 3-week backyard gardening project that produced raised dust clouds, I began feeling run-down, and a severe fatigue set in. Over a two-week period I developed a cough and fever. I was first diagnosed with bronchitis, and when antibiotics had no effect, a chest ex-ray was taken. I was diagnosed with pneumonia, and was prescribed a stronger antibiotic.
My health continued to decline, so a higher dose of the antibiotic was prescribed. By this time my symptoms included cough, fever, nausea, vomiting, drenching night sweats, skin lesions, joint and muscle pain, vision fluctuations, extreme fatigue, and muscle weakness. It hurt to bathe. It hurt to wear shoes. It hurt to be touched on my arms and legs. I did not have enough breath to speak a single sentence.
A chest CT scan was ordered, which revealed a mass in my left lung.
My doctor referred me to a pulmonary specialist, and ordered the Cocci titers blood test. Two weeks later the test results were in: I had Disseminated Coccidioidomycosis.
I sought out a local Valley Fever specialist. “Every Valley Fever patient’s rate of recovery is different,” said Dr. Craig Rundbaken, of the Respiratory & Valley Fever Clinic. The new plan of attack involved anti-fungal drugs, monthly titer and liver tests (the medication is hard on your liver,) chest x-rays, and plenty of rest.
Healing is a slow process. It’s been 8 months since my Valley Fever was diagnosed, and progress is good: many symptoms have disappeared, the mass in my lung has shrunk to 4.9cm (about 2 inches), and my blood titer levels continue to decline.
Want to know more?
The CDC website offers Valley Fever information.
The book, Valley Fever Silent Epidemic: The Common, Often Misdiagnosed Desert Ailment, by local expert Dr. Craig Rundbaken, offers information for both patients and healthcare professionals.
A YouTube channel is dedicated to sharing information about Valley Fever. You can watch the videos here.
An excellent paper on the Cocci spore, where it lives, and when it is most active, was written by Tom Volk of the University of Wisconsin. You can read his report online.
